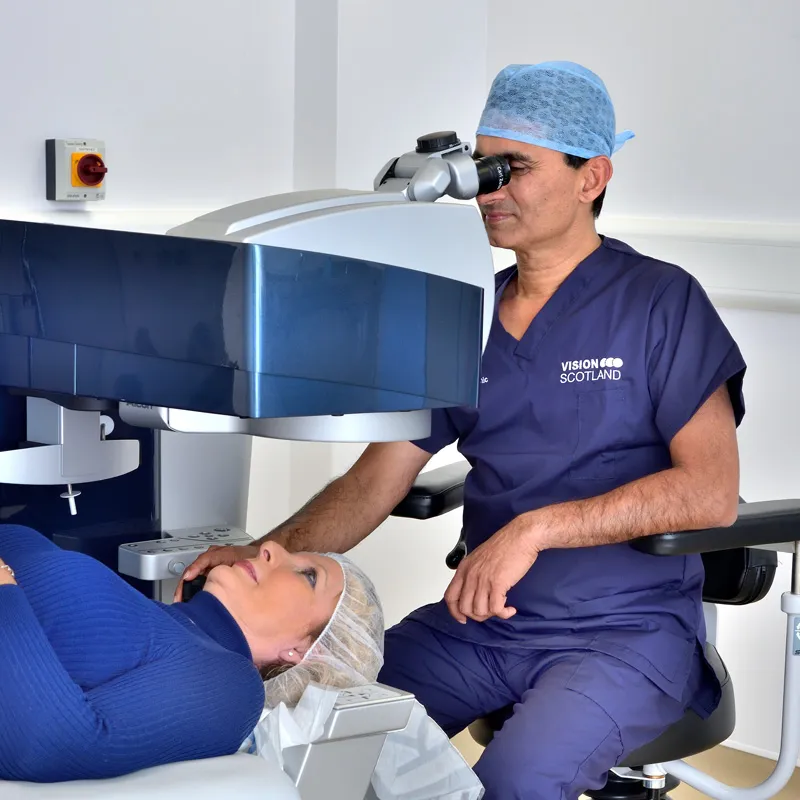
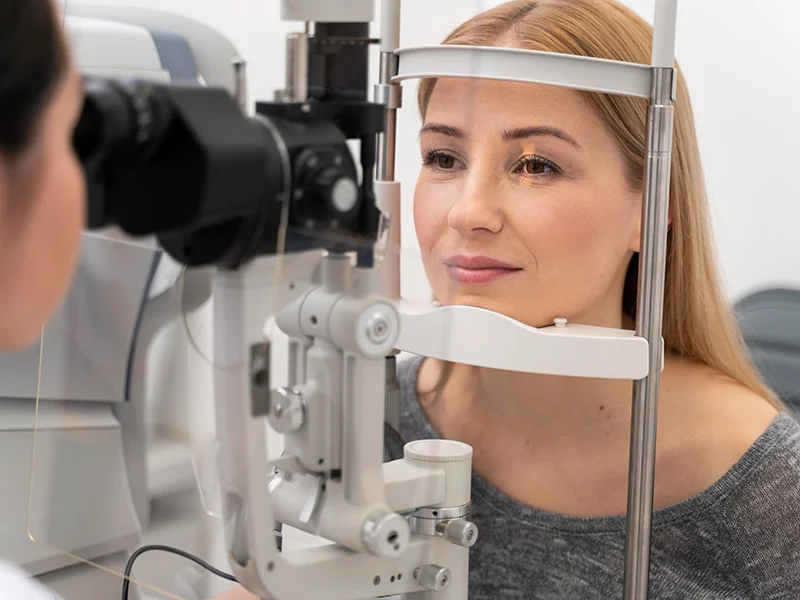
Patients who attend our clinic for cataract assessment are often very surprised to be recommended surgery to both eyes when only one eye is causing ‘problems’. Now, before we go any further, it is important to remember that you can only have cataract once. A cataract can not develop again after surgery. This conversation is therefore only relevant to patients who attend our clinic having not previously had any cataract surgery. Here we are going to outline the most common reasons for recommending surgery to both eyes when only one eye is the ‘problem’. No patient will ever be pressured into having surgery and will never feel forced to have both eyes treated. We will always give the best clinical opinion and advice and allow the patient to make an informed choice.
It is very common for patients to present with much poorer vision in one eye than the other. Patients will therefore often assume that the ‘good’ eye is functioning perfectly well and is not causing any issues. More often than not cataracts come as a pair and one needs to consider how the visual system will perform after having cataract surgery in one eye. In the case of a patient electing to have surgery on one eye when both eyes have cataract, there is a very high chance that what was previously the ‘good’ eye now becomes the ‘worse’ eye. This change can take a significant amount of time for the visual system to readjust to. Having both eyes treated means that the two eyes are immediately balanced and will be back working together much sooner as the contrast sensitivity will be equal. Contrast sensitivity – our ability to identify differences in shades and patterns. Sensitivity diminishes as cataract develops.
The visual system does not tolerate large differences in spectacle prescription between the eyes. It causes an imbalance. Any difference between the two eyes is known as anisometropia. Anisometropia can cause significant issues such as double vision when spectacles are worn and in such instances patients need to wear contact lenses to overcome this dilemma. For example, a 65 year old female attends the clinic with a prescription for shortsightedness (-8.00 both eyes). If surgery was to be performed in one eye aiming for excellent distance vision then the patient is going to struggle significantly after surgery when the untreated eye is still -8.00 and the other eye having had successful surgery has zero prescription. The patient simply would not tolerate this imbalance with spectacles and would therefore need to wear contact lenses. The other option would be to intentionally aim to leave the patient significantly short sighted after surgery but this of course means that the patient is just as dependent on spectacles after surgery that they were before surgery. Having surgery on both eyes immediately balances the vision and reduces/ eliminates the dependency on glasses or contact lenses after surgery.
Having both eyes treated allows for a much better chance of spectacle independence after surgery. Whilst this might not be important to everyone, for many people, the opportunity to reduce/ eliminate spectacle dependency is very appealing. Having both eyes treated allows for a patient to be considered for full vision correction using a trifocal lens. It also allows for use of a lens known as an extended depth of focus (EDOF) lens which is fast becoming a very popular choice for patients as it gives them not only very good distance vision without spectacles but
also very good intermediate vision which is perfect for those using the computer, reading music or seeing the dashboard in the car. Having two eyes treated can also allow for the surgeon to achieve monovision. Monovision is commonly employed by contact lens wearers and involves aiming for good distance in one eye and good near vision in the other eye.
There are numerous medical benefits of having a cataract treated even if one is achieving a reasonable level of vision. As a cataract develops, it reduces the amount of space in the anterior aspect of the eye and thus increases the risk of developing an eye condition called glaucoma. Those who are long sighted are at greater risk of this happening as the eye is naturally anatomically smaller. Removing the lens from the eye whether it has cataract or not, results in a lowering of the intraocular pressure (IOP). This technique is commonly employed in patients who have existing glaucoma as it can help with the long term management of the condition. Patients with a lazy eye are understandably hesitant about the need for surgery. They are less motivated to have surgery as the improvement in vision following surgery may be very minimal. A well developed, dense cataract is more difficult to remove and requires a greater amount of energy to be used during surgery and so it is easier and safer to remove a cataract at an earlier stage than a later stage. It is not sensible to simply leave a cataract forever even in a lazy eye as it could lead to blindness and a much more challenging surgery. For this reason, many patients with a lazy eye and significant cataract will be recommended to have surgery. If the cataract is less well developed then the need for surgery is less important but the cataract should be monitored annually for progression.
Cataracts only worsen over time and so postponing surgery is only delaying the inevitable. A proactive approach is to have the eye treated before symptoms become problematic.